Research Article - Der Pharma Chemica ( 2017) Volume 9, Issue 3
The Effect of Aromatherapy with the Essential Oil of Orange on Pain and Vital Signs of Patients with Fractured Limbs Admitted to the Emergency Ward: A Randomized Clinical Trial
Hekmatpou Davood*, Pourandish Yasaman, Varvani Farahani Pouran and Parvizrad RaminHekmatpou Davood, Traditional and Complementary Medicine Research Center (TCMRC), Arak University of Medical Sciences, Arak, Iran, Email: Hekmatpoudavood@gmal.com
Abstract
Background and objective: Pain is an emotional and unpleasant experience associated with actual or potential tissue damage. In this regard, this paper aims at studying the effect of aromatherapy with the essential oil of orange on patients with fractured limbs admitted to the emergency ward. Methods: 60 patients admitted to the emergency ward and then were divided in two groups of control and experiment by block method. 4 drops of the orange oil was poured on a pad and was pinned with a plastic pin to the patient's collar, about 20 cm distant from head. The old pad was replaced by the new one every 1 h. The patients' pain and vital signs were checked every 1 h for at last 6 h. The data were analyzed by SPSS21. Results: 40 (66.7%) patients were male and 20 (33.3%) were female. Their age average was 37.93 ± 18.19 years old. The most fractured cases were in the scapular (11 patients (18.3%)). Friedman test showed that pain in the experiment group (0.0001) increased significantly rather than the control group (0.339). There could be found no significant change between the two groups based on vital signs. Conclusion: Aromatherapy with orange oil can relieve pain in patients with fractured limbs but has no effect on their vital signs. Therefore, aromatherapy with orange oil can be used as a complementary medicine in these patients.
Keywords
Aromatherapy, Orange oil, Limb fracture, Pain, Vital sign, Emergency ward
Introduction
According to the definition by International Association for the Study of Pain (IASP), pain is an emotional or unpleasant experience associated with actual or potential tissue damage, or a description of a situation with such damage [1,2]. Pain relief by reducing transferring painful data to the central nervous system and optimizing analgesia treatment can reduce mortality and morbidity in patients [3-5]. Lack of pain control can activate the sympathetic nervous system and increase morbidity and mortality in patients. Indeed, the sympathetic system activities can increase myocardial oxygen consumption and lead to, in some cases, ischemia and even myocardial infarction (by decreasing oxygen due to coronary artery contraction and inhibition of local vasodilator mechanisms) [3-6]. Another important side effect of stimulation of the sympathetic nervous system id delay in stimulation of the digestive system (ileus) [3-7]. Impaired respiratory function in patients is the result of pain, especially in abdomen and thoracic, is one of the consequences of lack of proper pain management in patient [7]. Moreover, pain has psychological effects as well, and is regarded as the main reason for fear, anxiety, distress, and disappointment [8]. There are different ways to control pain, including systemic analgesics (narcotics and non-narcotics) and local anesthesia techniques, each can be prescribed according to the patient's medical condition [9]. A safe way that can control the pain with no side effects such as respiratory problems, pruritus, or hemodynamic clutter is ideal [10].
Fractures and orthopedic surgery cause severe pain in patients and we will have to use narcotic analgesics [11-16]. Since the narcotic analgesics have general side effects such as respiratory problems, sedation, nausea and vomiting, symptoms of tolerance or withdrawal syndrome in patients, using nonpharmacological methods as complement rather than alternative interventions are recommended. In this regard, there are methods in complementary medicine by which nurses can help patients [17,18]. Since the narcotic analgesics have general side effects such as respiratory problems, sedation, nausea and vomiting, symptoms of tolerance or withdrawal syndrome in patients, and they need to be prescribed by a physician or, in some cases, nurses avoid prescribing them due to fear of side effects or make longer the time between doses, using pharmacological methods can be helpful and more efficient than non-pharmacological methods [19]. Aromatherapy is the controlled use of natural aromatic oils to enhance psychological and physical well-being and is used as a part of nursing in many countries including Switzerland, Germany, England, Canada, and America [20]. The aromatic oils are extracted from aromatic plants, which are anti-inflammatory, antimicrobial, and reduce pain and stress [20-23]. In fact, aromatherapy is the second complementary method among nurses with most clinical applications [24]. It has been proved that inhalation of the essential oil of orange can reduce the labor pain [25]. It also can stimulate the central nervous system, enhance moods and causes sedation and relief, is antispasmodic, anti-inflammatory, anti-bloating, digestive, and diuretic and can lower the blood pressure. Its active substances are limonene, and Flanders Citral (Levomenthol) [26,27]. Massage and aromatherapy with a combination of ginger and orange oils was effective in relieving knee pain in the first week [28]. A study has shown that edible oil of orange can reduce breast pain caused by premenstrual syndrome [29].
Considering the importance of pain and proper management of pain in patients and few researches on the relationship between aromatherapy and pains of fractured bones, this paper aims at studying the effect of aromatherapy with the essential oil of orange on pain and vital signs of patients with fractured limbs admitted to the emergency ward.
Methods
This research is a clinical trial registered in the Center of Clinical Trial in Iran under code IRCT201607124519N6. Samples size was obtained by the following formula.
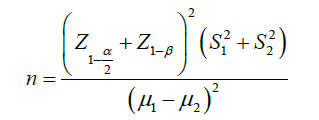
According to the comparison of means formula and reference [30], the sample size for each group was evaluated as 30. In the emergency ward of Vali-e-Asr Hospital, 60 patients were selected by the purposive sampling method and were divided in two 30- patinet groups of experiment and control by block method. The collecting data tolls were a demographic questionnaire, self-report pain scale measured by the 10-item Visual Analog Scale (VAS). The vital signs were checked by the researcher of that shift. This research was done in one shift work (morning or afternoon).
The patients were fractured limbs admitted to the emergency ward of Vali-e-Asr hospital in Arak, who must do orthopedic surgery voluntarily participated in this trial (they were matched based on their age, sex, type of fracture, and the initial pain). For intervention, 4 drops of the essential oil was poured on the pad and was pinned with a plastic safe pin to the patients' collars with about 20 cm distant from the head, and the pads were replaced with new ones every 1 h. The pain and vital signs in patients were checked every 1 h for at last 6 h. Since aromatherapy was used as a complementary medicine, the common treatments in the ward have been performed to control the pain.
Inclusion criteria
Patients over 18 years old, with no history of chronic pain, vision problems, respiratory problems, asthma, allergy, and with mental and smell health could participate this research. The informed consents were obtained from the participants.
Exclusion criteria
Lack of interest in participating or withdrawing while performing the research, and having any allergic symptoms while performing the research.
Collecting data tools
The visual analog scale (VAS 0-10) was used to evaluate the pain.
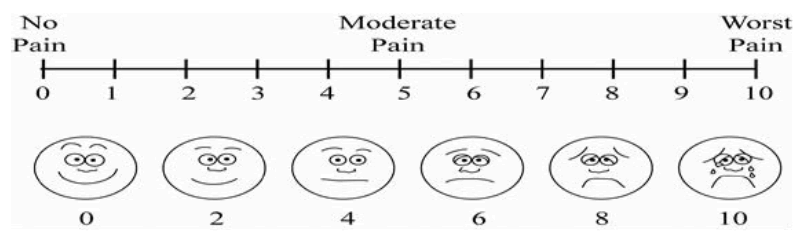
This scale is graded between 0-10; 0 shows no pain and 10 implies the most severe pain. The patients show their pain by pointing on the right scale. This scale allows the patients to show their pain freely [31].
This scale is the most widely used pain evaluation tool in the world. In addition to validity and reliability, this tool is easy to use. Zero, in this scale, shows no pain, 1-3 show mild pain, 4-6 moderate, 7-9 severe and 10 indicates very severe pain [32].
Many studies out of Iran have proved its validity and reliability [33]. In Iran, the reliability of this scale was confirmed with correlational coefficient 0.88 [34].
Results
60 patients were participated in this research, 30 in the intervention and 30 in the control group. 40 (66.7%) patients were male and 20 (33.3%) were female. Their age average was 31.93 ± 18.19 years old; the youngest was 18 and the oldest patient was 72 years old. 37 patients (61.7%) were married and 23 (38.3%) were single. 11 patients (18.3%) had diploma, 8 (13.4%) had academic studies and 41 patients (68.3%) had lower grades. The subjects in the two groups have the same demographic information and there could be found no significant differences
Fisher's exact test results showed that the distribution of fractures in the two groups have no significant difference. Although the most common fractures were of the scapula with 11 patients (18.3%) (Table 1).
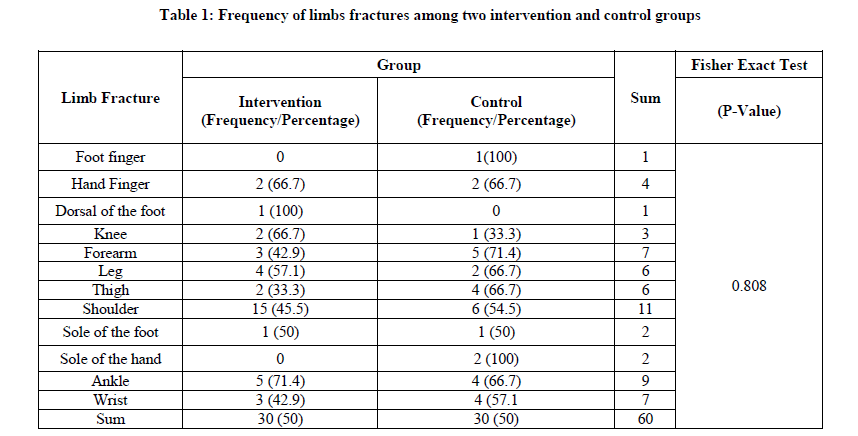
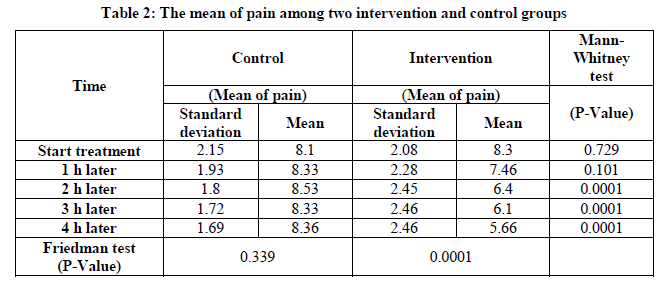
The results showed no significant statistics difference in mean pain scores in different times. But pain scores in the intervention group have significant differences at different times (P Value=0.0001), and with increasing duration of pain was significantly reduced (Table 2).
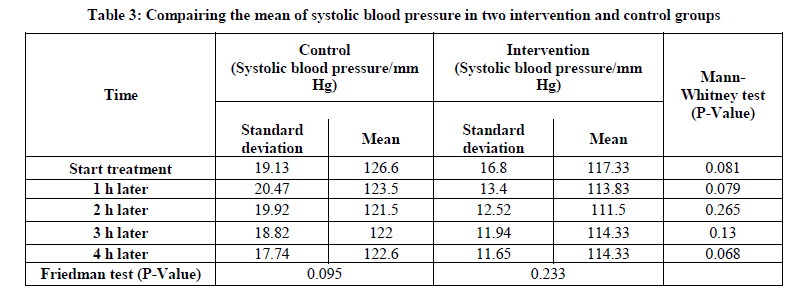
The results showed that at all times no statistically significant difference in mean of systolic blood pressure. This means that changes in systolic blood pressure in both groups did not differ at different times (Table 3).
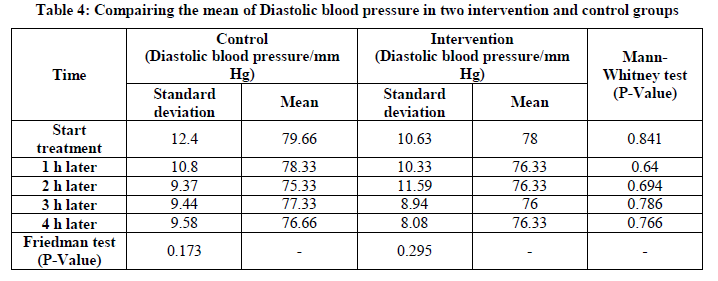
The results showed that at all times no statistically significant difference in mean of diastolic blood pressure. This means that changes in diastolic blood pressure in both groups did not differ at different times (Table 4).
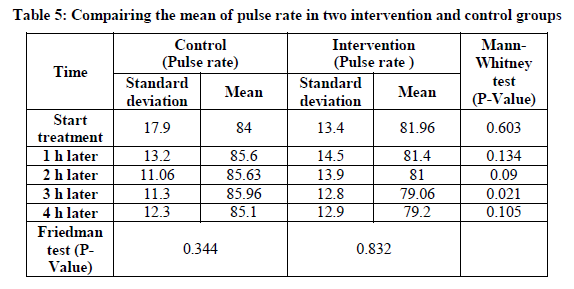
The results showed that in all times but 3 h after the intervention, the mean heart rate in both groups was not statistically significant. This means that changes the pulse in both groups did not differ at different times (Table 5).
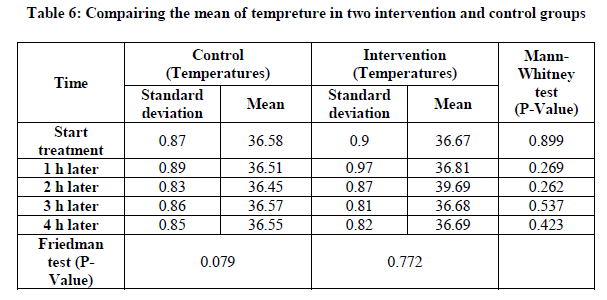
The results showed that at all times no statistically significant difference in mean of tempereture. This means that changes in tempereture in both groups did not differ at different times (Table 6).
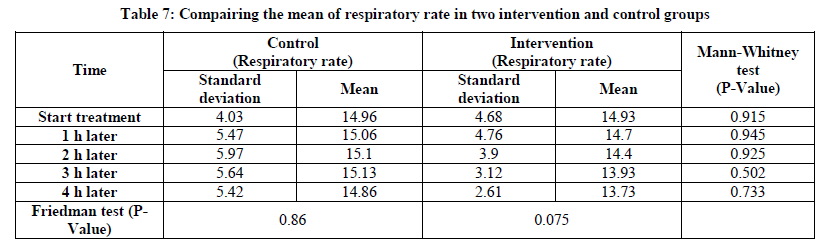
The results showed that at all times no statistically significant difference in mean of respiratory rates. This means that changes in respiratory rates in both groups did not differ at different times (Table 7).
Discussion
The results showed that the pain averages the control and experiment groups before intervention were 8.3 and 8.1, respectively, which show severe pain. This result conforms to the results by the previously done researches that revealed high severity of orthopedic pains [11-16]. Also, the results of this paper showed that severity of pain in the two groups of experiment and control was not significantly different. Fractures in limbs result in severe pains that make the treatment team to use narcotic analgesics [11-16].
The results of this paper showed that changes in pain severity in the intervention group have significant statistical differences at different times; over time, the pain reduced significantly in the intervention group. These findings indicate the positive effect of the essential oil of orange on pain relief in the patients with orthopedic fractures, which are in line with the results by Lehrner on dental procedures [35]. Yip et al. showed that aromatherapy and massage with orange oil and ginger can reduce knee arthritis pains [28], conforming to the results of this paper. However, Malachowska studied the pain from the Lancet to measure blood sugar in children with type I diabetes [36] and obtained results different from the results in this paper; this difference may be due to difference in pains in orthopedic fractures and lancet. Ozgoli showed that the orange oil can relive the pain in breasts caused by premenstrual syndrome [29]. Fakari also showed that the orange oil can reduce labor pain, which is in line with the results of this paper [25].
Another main objective of this paper was studying the effect of the orange oil on vital signs such as pulse rate and respiration, blood pressure, and body temperature in patients with fractured limbs admitted to the emergency ward. There could be found no significant difference between the vital signs in the two groups at different times, which indicates different results with those obtained by Jafarzade et al. [37]. Jafarzade showed that inhalation of the orange oil decreased the heart rates in the children who had referred to dentist; this difference may be due to difference in the natures of dental procedures and fractures. Moreover, the atmosphere in the emergency ward, e.g. crowdedness, long waits for surgery and fear of the future, may reduce the effect of the orange oil on the patients' vital signs. The limitation of this study was lack of enough information about the complementary medicine by the patients, which could affect the results of effects of inhalation of the orange oil on the patients' vital signs in the study.
Conclusion
Aromatherapy with the essential oil of orange as a complementary medicine could relieve pain in patients with fractured limbs before surgery. It can lead to faster recovery and discharging of patients as well as reduce the costs of hospitalization. In this context, aromatherapy with the orange oil in patients with fractured limbs is recommended.
Ethical Considerations
This project has been registered under code IR.ARAKMU.REC.1395.111. The personal characteristics of all subjects of the research have been kept confidential. All participated voluntarily and the informed consents were obtained. The subjects could withdraw whenever they wanted.
Acknowledgment
We here thank Traditional and Complementary Medicine Research Center (TCMRC) in Arak University of Medical Sciences, the personnel in the emergency ward of Vali-e-Asr Hospital in Arak and all the patients who participated in this project.
References
[1] A.B. Shang, T.J. Gan, Drugs., 2003, 63, 855-867.
[2] M. Agah, A. Dabbagh, M. Hashemi, Pajoohande., 2006, 11, 149-152.
[3] Kehlet, K. Holte K, Br. J. Anaesth., 2001, 87, 62
[4] S. Liu, R.L. Carpenter, J.M. Neal, Anesthesiology., 1995, 82, 1474.
[5] H. Kehlet, 3rd edn. Philadelphia, Lippincott-RavenPublishers, 1998.
[6] J.P. Desborough, Br. J. Anaesth., 2000, 85, 109.
[7] M.D. Fratacci, W.R. Kimball, J.C. Wain, Anesthesiology., 1993, 79, 654.
[8] K. Naghibi, Isfahan: Mani pub, 2001.
[9] American Society of Anesthesiologists, Anesthesiology., 1995, 82, 1071.
[10] J. Lim, J. Brainres, 2006, 1123, 80-88.
[11] C. Stein, Engl. J. Med., 1995, 332, 1685-1690.
[12] B.O. Ogunnaike, S.B. Jones, D.B. Jones, D. Provost, C.W. Whitten, Anesth. Analg., 2002, 95(6), 1793-1805.
[13] E. Marret, O. Kurdi, P. Zufferey, F. Bonnet, Anesthesiol., 2005, 102(6), 1249-1260.
[14] L.S. Nuutinen, J.O. Laitinen, T.E. Salomaki, Drug. Saf., 1993, 9(5), 380-393.
[15] E. Meet, Drugs., 1992, 5, 14-29.
[16] H. Kehlet, J.B. Dohl, Drug., 1992, 44, 38-41.
[17] J.W. Ball, R.C. Bindler, K. Cowen, 2nd edn., Pilladelphia: Prentice Hall, 2010.
[18] R. Steolting, R. Miller, 5th ed., Philadelphia: Churchill Livingstone Elsvier, 2007, 112-122.
[19] J.H. Marilyn, W.D. Wong’s 8th ed. Louis, MO: Mosby/ Elsevier 2009, 194-198.
[20] J. Buckle, J. Assoc. Nurs. AIDS. Care., 2002, 13(2), 81-99.
[21] L. Long, A. Huntley, E. Ernest, Complement. Ther. Med., 2001, 9, 178-185.
[22] B. Cooke, E. Ernest, Br. J. Gen. Pract., 2000, 50, 493-496.
[23] A.L. Howarth, Compl. Ther. Nurs. Midwifery., 2002, 8, 138-141.
[24] S. Marline, K. Laraine, Lippincott., 2008, 22(1), 3-9.
[25] R.F. Fakari, M. Tabatabaee Chehr, F. Rashidi Fakari, H. Mortazavi, H. Kamali, V. Tayebi, J. North. Khorasan. Univ. Med. Sci., 2013, 5(2), 363.
[26] A. Soltani A, 2nd edn., Tehran: Arjmand, 2005, Persian.
[27] A. Haji Akhondi, N. Baligh, Tehran: Islamic Azad University, 2005, Persian.
[28] B. Yip, C.H. Tam Ch, Compl. Ther. Med., 2008, 16, 131-138.
[29] G. Ozgoli, S. Esmaeili, N. Nasiri, J. Reprod. Fert., 2011, 12(2), 123-129.
[30] M. Kanani, S.R. Mazloum, A. Emami, N. Mokhber, Quarterly J. Sabzevar. Univ. Med. Sci., 2012, 19(3).
[31] G.A. Hawker, S. Mian, T. Kendzerska, M. French M, Arthritis. Care. Res., 2011, 63, 11: S240-52.
[32] G. Mendelson, T.S. Selwood, J. Behav. Assessment., 1981, 3(4), 263-269.
[33] E.R.Vickers, M.J. Cousins, A. Woodhouse, Aust. Dent. J., 1998, 43(6), 403-439.
[34] M. Rezvani Amin, M. Siratinayer, A. Ebadi, T. Moradian, Qom. Univ. Med. Sci. J., 2012, 6(1), 31-34.
[35] J. Lehrner, C. Eckersberger, P. Walla, G. Pötsch, L. Deecke, Physiol. Behav., 2000, 71(1-2), 83-86.
[36] B. Małachowska, W. Fendler, A. Pomykała, S. Suwała, W. Młynarski, J. Pediatr. Endocrinol. Metab., 2016, 29(1), 47-53.
[37] M. Jafarzadeh, S. Arman, F.F. Pour, Adv. Biomed. Res., 2013, 6, 2, 10.



